Diabetes awareness month is the month of November. London has been doing its part in researching and finding better ways for diabetic patients to cope with their illnesses.
Some diabetic patients have a hard time regulating their blood glucose levels. This prompts them to inject insulin on a daily basis to keep those levels up and basically survive. Where did this idea of a drug that could save thousands of lives come from?
Insulin was actually co-discovered right in London Ontario.
“Frederick Banting is Canada’s co-discoverer of insulin. His importance to London is undeniable,” said Grant Maltman, curator of the Banting House museum.
Maltman says in 1921, Banting came to the idea of insulin after reading a few articles on the pancreas and then going to bed.
“Banting was fortunate to take a job at Western University at the medical school. He’s asked to give the pancreas and diabetes and it was a subject he admitted to knowing very little about. He reads a number of articles to prepare his lecture, retires for the evening, reads an article on diabetes while he’s in bed, and at two o’clock in the morning the idea comes to him.”
The first human trial of insulin failed, but some altercations in the drug made it something for diabetics to rely on even today.
Present Research
Dr. Subrata Chakrabarti is the chair of pathology and lab medicine at Western University. He started researching for diabetic cures after a personal connection with the disease.
“My father was diabetic and then for some time I worked at a hospital who focused on diabetic retinal damage and that sort of started my interest in it.”
He has his own lab where he researches mechanisms to combat chronic diabetic illnesses.
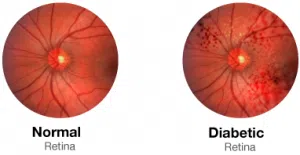
“In my lab, we look at how diabetes causes damage to the tissue. Mainly we focus on retina, which is the tissue in the back of the eye. We also focus on the kidney and heart.”
Chakrabarti is currently looking into what mechanisms of diabetes cause chronic illnesses. By blocking bad protein cells, they can potentially prevent diabetic illnesses from even occurring.
“If we can block some of them, we can prevent more production of bad proteins to prevent chronic illnesses.”
He hopes in the future he can take his research and apply it to real patients so that diabetic patients don’t ever have to go through what his dad did in the past.
Half of all limb amputations in Ontario alone are directly related to diabetes. Down at St. Joseph’s Family Medical and Dental Centre, nurse practitioner Betty Harvey has put together a new tool called “FURST” to significantly reduce diabetes related amputations.
“FURST stands for foot ulcer risk stratification tool.”
The tool is designed for family doctors to identify diabetic foot ulcers in a seamless way.
“This is for a busy clinician to take what they know, structure it and stream it down into just the really key things that you need to look at on that foot. Then take the cluster of presentation in that person’s foot, attach it to a risk score, and then using this tool, the risk score tells the doctor right where to send the patient,” said Harvey.
80% of all diabetic patients are dealt with at family doctor medical centres. Harvey says this tool is all about a quicker way for doctors to diagnose a diabetic patients’ illness before it is too late.
“Any tools that help make it streamline and simple and sort of shrink the amount of complication that it is to diagnose that at risk-foot, that’s what it’s all about.”
From Frederick Banting almost 100 years ago, to Subrata Chakrabarti, to Betty Harvey, London is no doubt doing its part in combatting the deadly disease that diabetes is.